What is ePHI ? Challenges, Best practices, and Strategies
Explore ePHI protection in healthcare: its significance, HIPAA's role, challenges, best practices, and advanced strategies to ensure top-tier ePHI security
Electronic Protected Health Information (ePHI) refers to PHI that is created, stored, or transmitted electronically. It is a subset of PHI, Protected Health Information which is regulated in the United States by the Health Insurance Portability and Accountability Act of 1996, known as HIPAA.
ePHI is extremely sensitive information and a recurrent target for bad actors. Federal records show that healthcare breaches exposed 385 million patient records from 2010 to 2022.
We don’t want you to become this statistic.
That’s why we’ve updated this guide. We’ll cover what ePHI is and what it isn't, what you need to know about HIPAA and ePHI compliance, and we’ll share the best practices for ePHI protection, along with some challenges you may encounter in your safeguarding path.
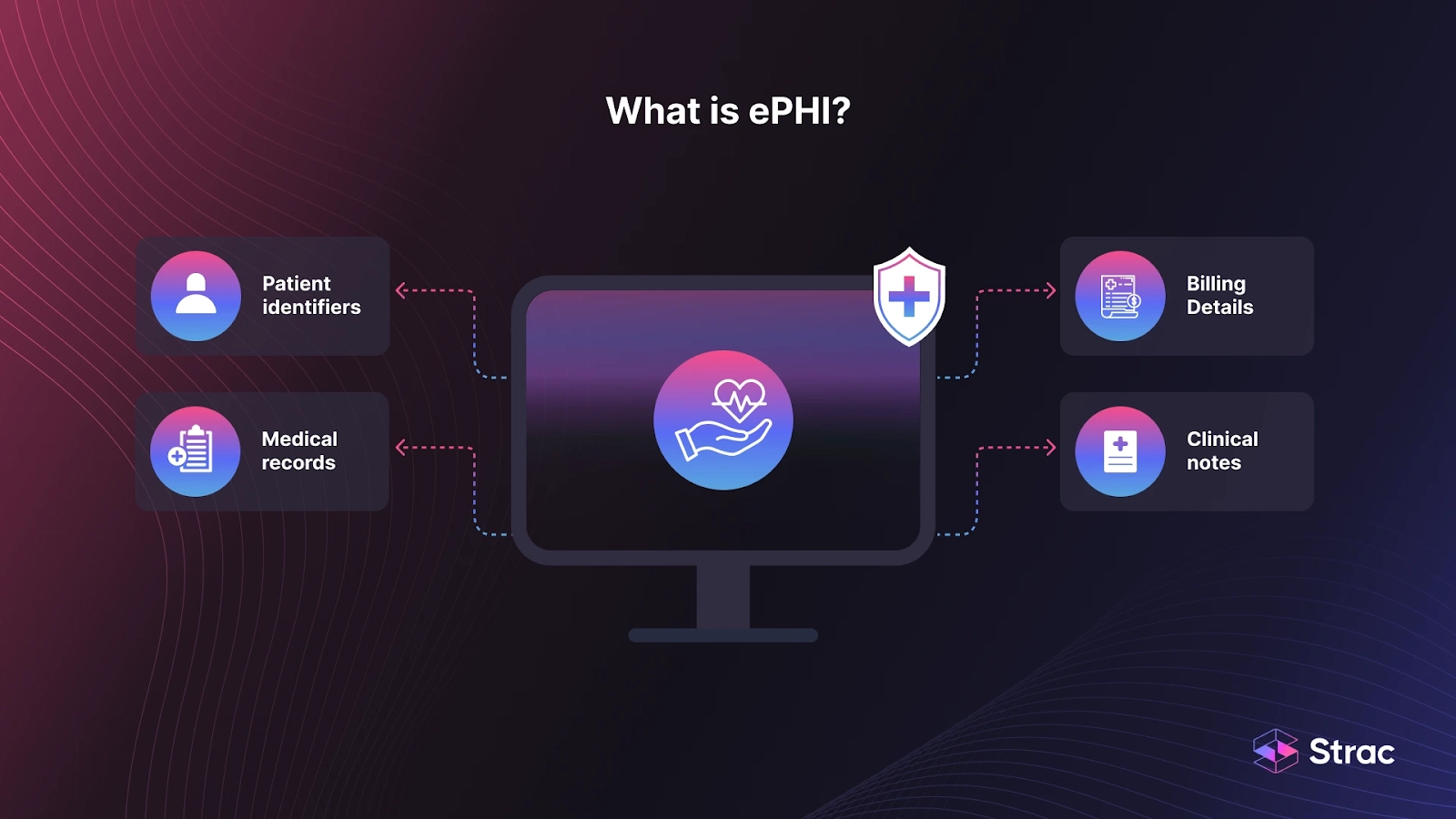
Electronic Protected Health Information (ePHI) refers to all Protected Health Information (PHI) that is created, stored, transmitted, or received electronically. Under HIPAA, any information that can identify a patient is considered PHI—so ePHI is simply PHI in digital form. This includes:
HIPAA defines 18 specific identifiers that qualify as ePHI when linked to health data. These include common ones like name, email, and SSN—as well as less obvious examples like IP addresses, biometric data, and vehicle IDs.
The main takeaway is that if it can identify a patient, it’s ePHI.
To help clarify what qualifies as ePHI, the table below provides practical examples. If unsure, consult the 18 HIPAA identifiers—any of which, when linked to health data and stored or transmitted electronically, constitute ePHI.
What Is ePHI?
ePHI (electronic Protected Health Information) is any health-related data stored or shared digitally that can be linked to a specific person; for example, a patient’s medical record number in systems like EPIC, an email with their name and diagnosis, a cloud-stored lab result tied to their name and date of birth, or billing records with SSN and insurance details. On the other hand, information is not considered ePHI if it cannot identify an individual, such as anonymous blog posts, fully de-identified lab results, synthetic datasets, personal wearable data only accessible by the user, standalone IP addresses, or physician notes without patient identifiers.
ePHI is distinct from other types of electronic data in four key ways:
We’ve established what ePHI is (and isn’t), and why it’s so critical. Before exploring how to protect ePHI and best practices, let’s look at how HIPAA regulates ePHI and what compliance requires.
Here is the list of all the components of ePHI as defined by the U.S. Department of Health & Human Services (HHS) under the HIPAA Privacy Rule

The Health Insurance Portability and Accountability Act of 1996 (HIPAA) directed the U.S. Department of Health and Human Services (HHS) to create regulations protecting the privacy and security of health information. HHS established three key rules that apply to ePHI:
(Standards for Privacy of Individually Identifiable Health Information)
This rule sets national standards to protect individuals’ medical records and other personal health information. It applies to all forms of PHI—whether electronic, paper, or oral—and governs how covered entities may use and disclose this data.
(Security Standards for the Protection of Electronic Protected Health Information)
This rule provides a framework for safeguarding ePHI when it is stored, accessed, or transmitted electronically. It outlines three categories of security safeguards: administrative, physical, and technical.
This rule requires covered entities and business associates to notify affected individuals, HHS, and—in some cases—the media when unsecured ePHI is breached. Notification must occur without unreasonable delay and within 60 days of discovery.
A breach of ePHI often leads to a HIPAA violation. Not all violations are equal, however. Our HIPAA compliance guide explains the four tiers of HIPAA violations based on the level of culpability—from unintentional lapses to willful neglect. Spoiler alert: Tier 4 violations carry the most severe civil penalties. In extreme cases, separate criminal penalties may also apply.

To comply with HIPAA’s Security Rule, healthcare entities must implement safeguards that ensure the confidentiality, integrity, and availability of ePHI—known as the CIA triad.
Below are eight core components to review for HIPAA Security Rule compliance. Our PEC framework—Plan, Enable, Control—provides a structured approach to managing these responsibilities:
As healthcare becomes increasingly digital, protecting ePHI feels like hitting a bullseye on a moving target–that moves faster and faster. There are three key challenges to keep in mind when protecting ePHI:
Healthcare organizations often rely on third-party cloud services, which can limit control over data. Risks include unauthorized access (especially in multi-tenant systems), accidental data loss, and complex HIPAA compliance. If misconfigured, cloud environments can expose sensitive data. The average cost of a healthcare data breach reached $10.1 million in 2022. This is why cloud data loss prevention is a must.
Cybercriminals use phishing to target employees, while ransomware attacks surged from 34% in 2021 to 60% in 2023. Insider threats—both accidental and malicious—remain common. In one case, a New York medical center faced a $3 million fine after losing an unencrypted laptop and flash drive. Unsecured mobile devices are frequent sources of ePHI exposure.
Old or unused data increases breach risk and may violate retention rules. Stale data can also undermine the accuracy of current records. Critically, deleting files doesn’t ensure secure removal—only certified wiping or destruction meets HIPAA disposal standards.
Learn more about sensitive data categories in the Strac Catalog of Sensitive Data Elements.
It’s all about protocols. Protecting ePHI requires layered safeguards that address its full lifecycle—from creation and transmission to storage and deletion. Below are three essential focus areas for maintaining HIPAA compliance and protecting sensitive health information:

Review our detailed DLP Security Checklist.
When it comes to security and compliance, it’s always worthwhile to go the extra mile. While basic compliance with regulations like HIPAA is essential, the following advanced strategies can ensure more robust ePHI protection.

Strac is a data loss prevention (DLP) solution, dedicated to safeguarding ePHI from unwarranted breaches and cyberattacks. Its core features include:
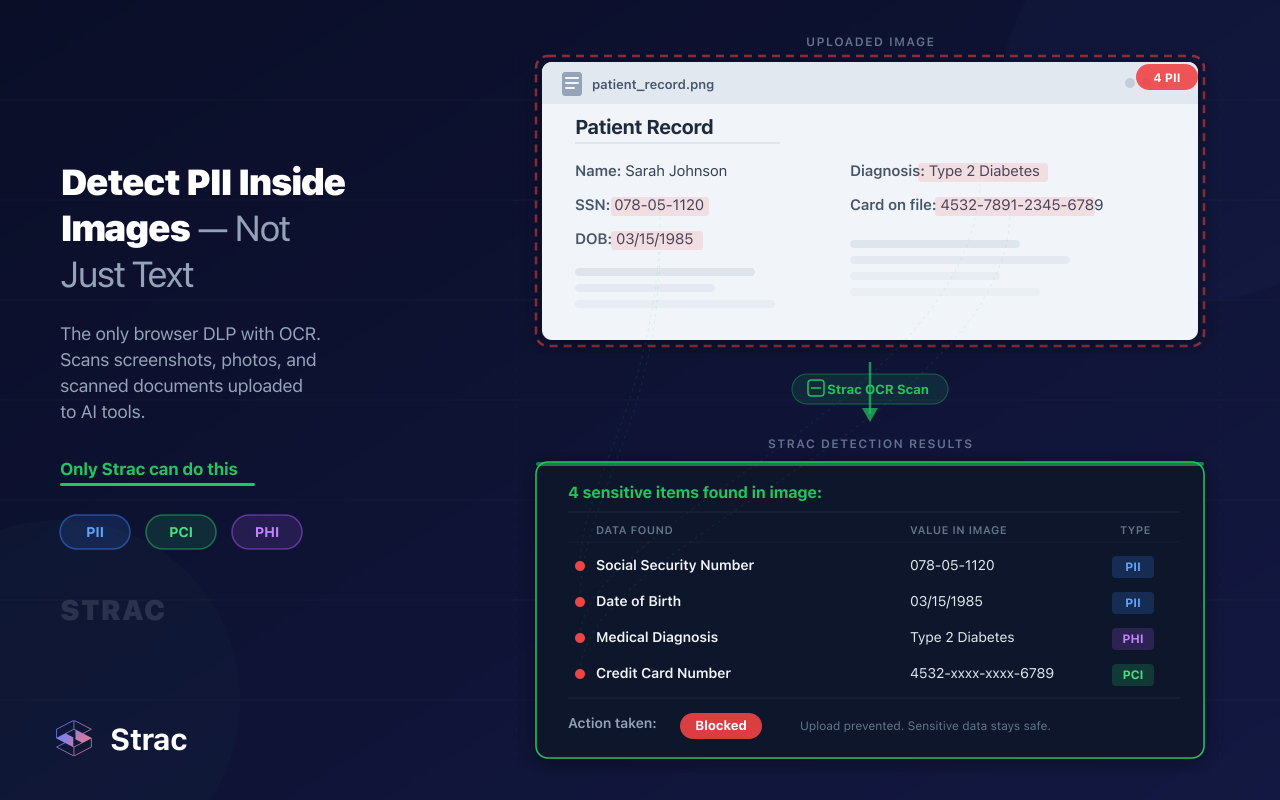
By now you should have a solid understanding of what ePHI is, how it is regulated by HIPAA, and the best practices to protect your ePHI and ensure HIPAA compliance. For further reference, we recommend you check out HIPAA PHI Guide, the basics of Data Loss Prevention (DLP), and how to encrypt email in Outlook.
And remember, here at Strac.io we obsess over ensuring proper data loss protection across all vectors and we are here to help, so book a demo today.

ePHI stands for Electronic Protected Health Information—any patient-identifiable health data created, stored, or transmitted electronically under HIPAA.
Medical records, billing info, email addresses linked to diagnoses, and IP addresses collected during telehealth visits all qualify.
Covered entities and business associates, including healthcare providers, insurers, and vendors handling patient data, must follow HIPAA’s ePHI regulations.
.avif)
.avif)
.avif)
.avif)
.avif)






.gif)

